Category: general
-

What Actually Changes After ACL Surgery
We recently had a staff meeting and were discussing our ACL Vald metric data and how we interpret it for our patients. As you know, there’s a ton of research on ACL rehab, but not a lot that actually tells you what’s happening week to week and across the full first year in the same…
-
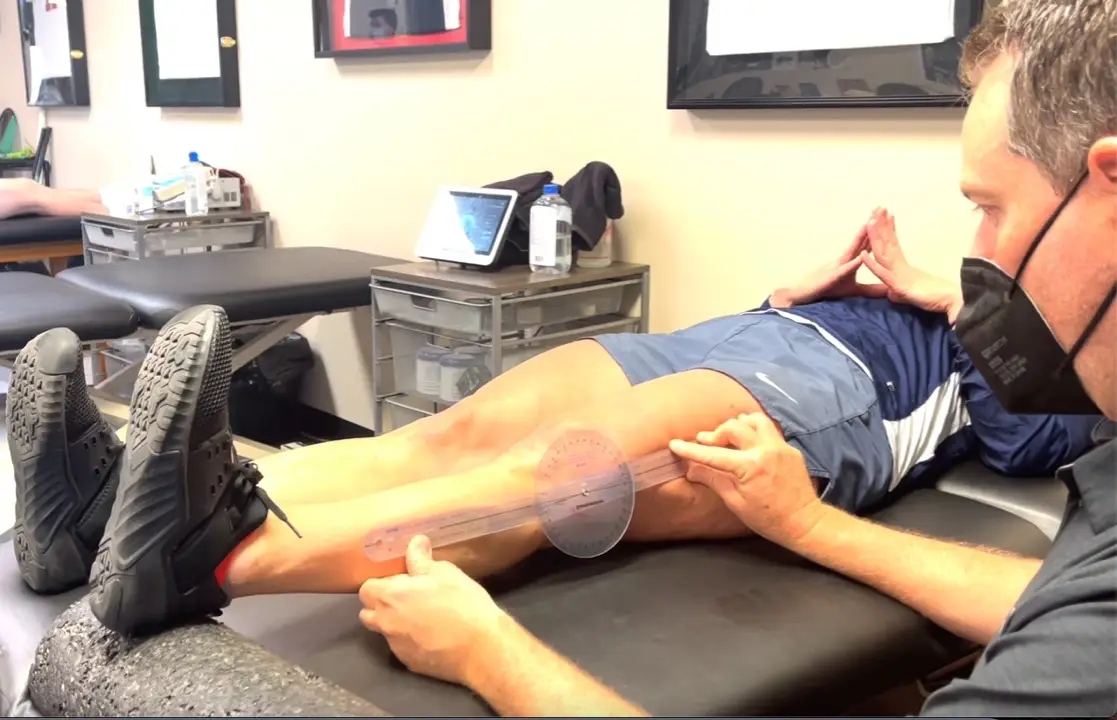
Simplifying ACL Rehab
—
by
ACL surgery continues to be a huge focus in the literature and in our outpatient rehabilitation settings. Numerous studies focus on return to play guidelines and retear rates. Social media is all over the place, most times. Let’s try to make things simple and set the stage early. Paralysis by Analysis- What ACL tests are…
-
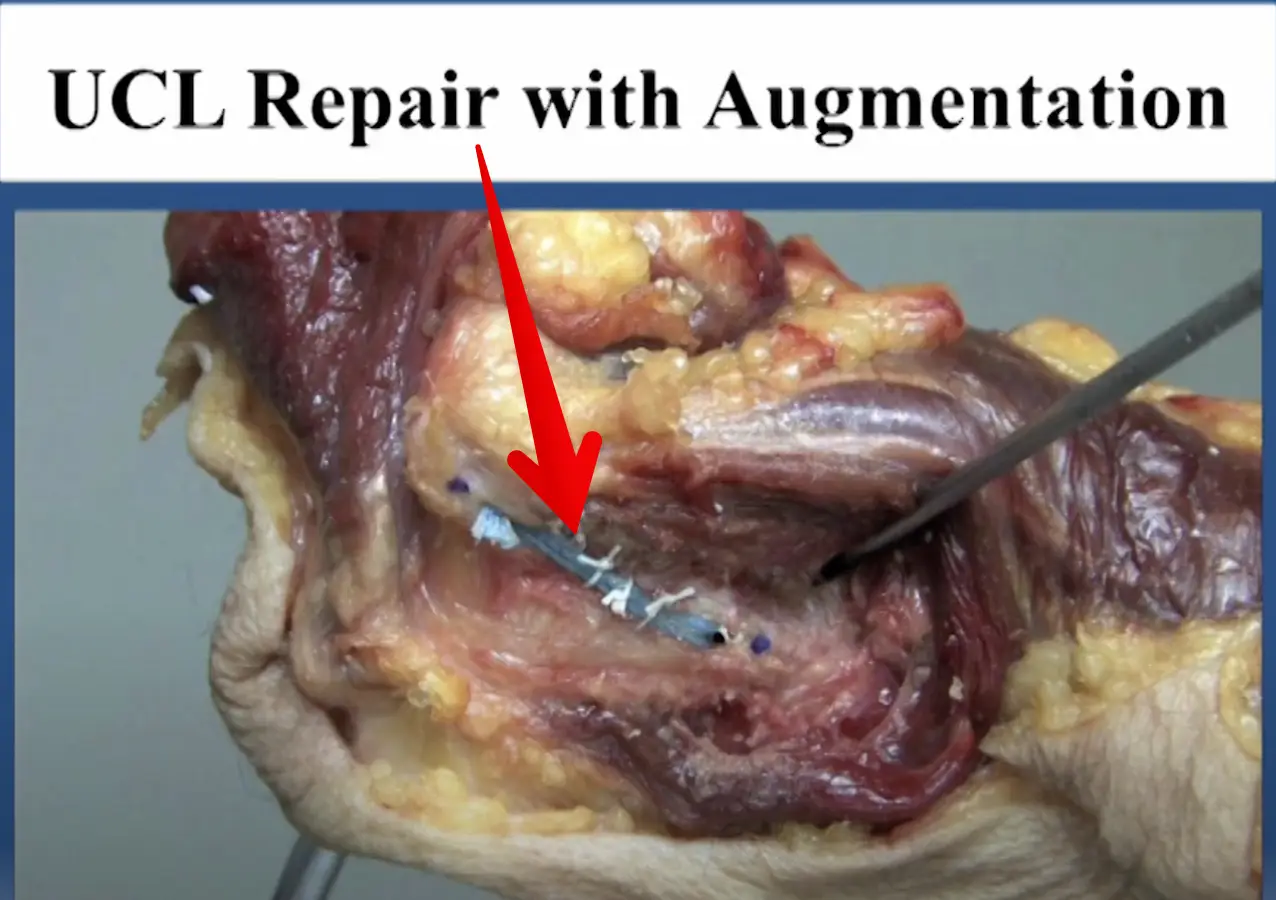
Diagnosed with an elbow UCL Tear- Reconstruction or Internal Brace surgery?
—
by
So, you’ve been diagnosed with a UCL tear in your elbow and your world has been turned upside down. Have no fear, many have been there before you and have done pretty well. But now, there’s a new option for elbow surgery and you’re not sure if it’s right for you. I hope this post…
-
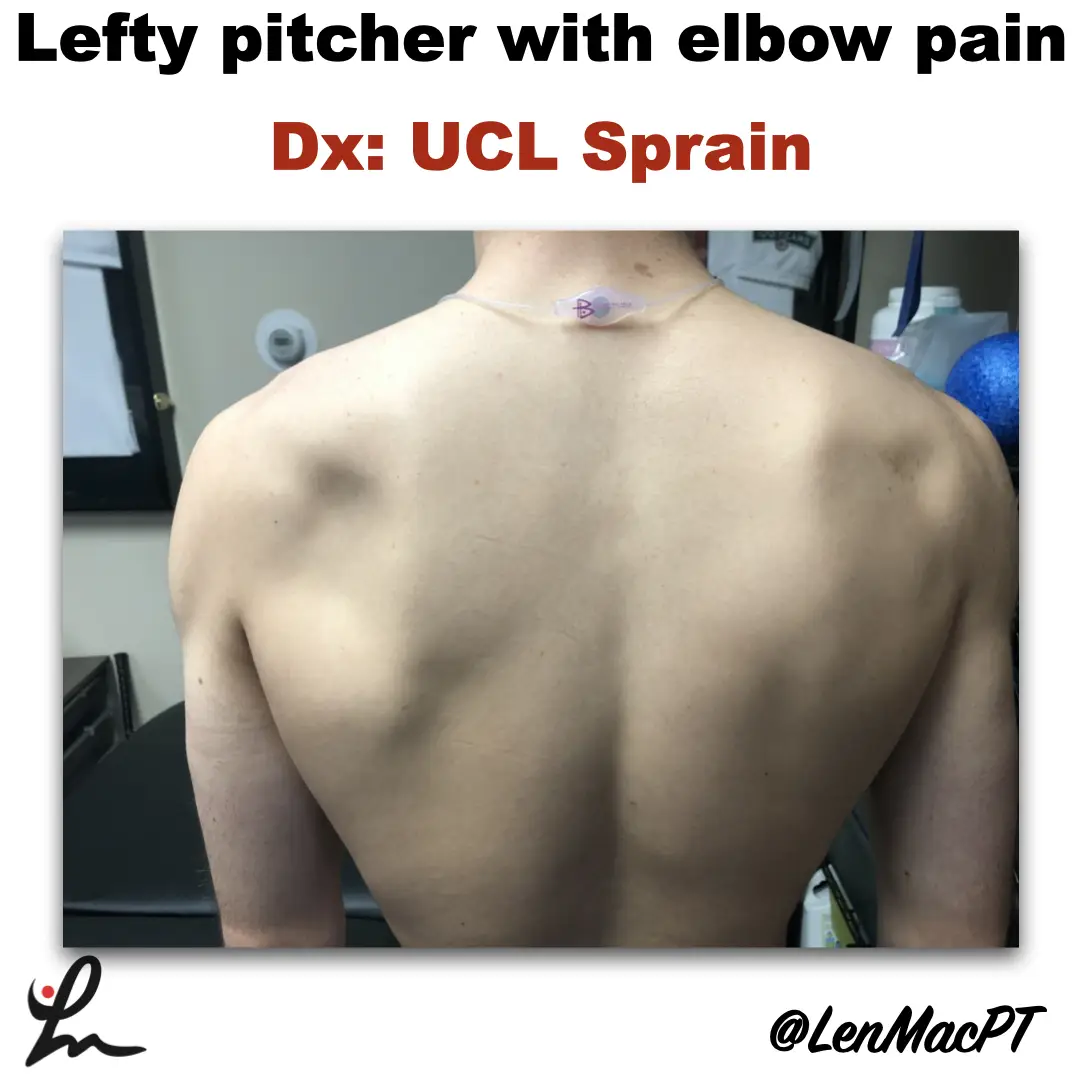
Infraspinatus atrophy in a baseball pitcher with a UCL sprain
—
by
Infraspinatus atrophy due to a spinoglenoid notch cyst This was an incidental finding of mine in a collegiate baseball pitcher. He presented with a UCL sprain during his senior year and was struggling. He came in looking to salvage his senior year and attempt to pitch at some point. UCL surgery would’ve been warranted if…
-
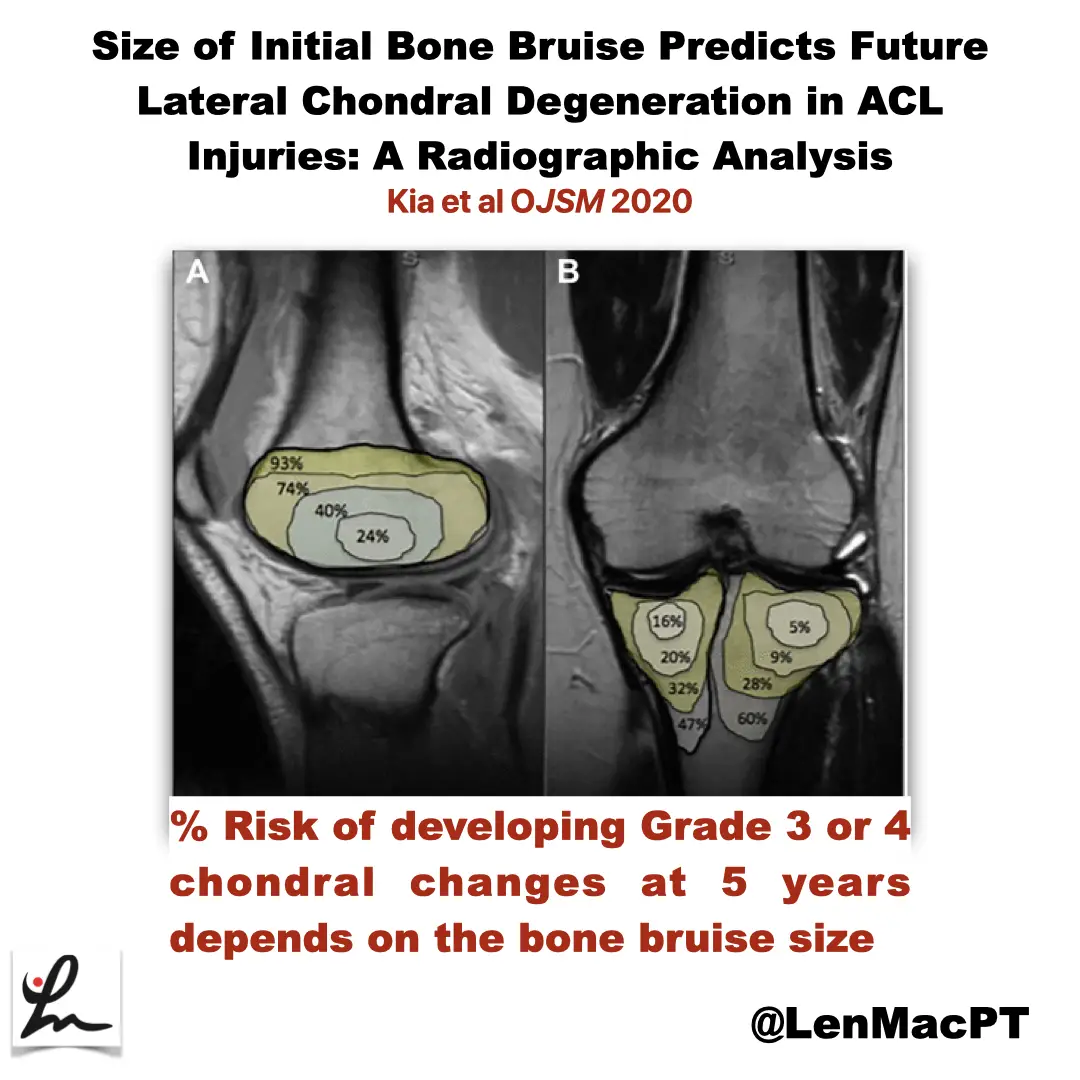
ACL tears and bone bruises
—
by
Research Review Not sure if you saw my recent post on social media about bone bruises after an ACL tear so I wanted to discuss it further here. In this study, the authors looked at the incidence of radiographic chondral changes (without correlation with clinical and functional outcomes) on MRI 5 years after the ACL…
-
Risk Factors for Recurrent Instability After a Bankart Repair Surgery
—
by
Recurrent instability after a Bankart repair surgery is unfortunately very common. This paper looks to highlight the most common risk factors associated with recurrent instability. I thnk it’s valuable to understand these various risk factors so you can better educate your patients. It may also help clinicians be mindful of the people that may need…
-
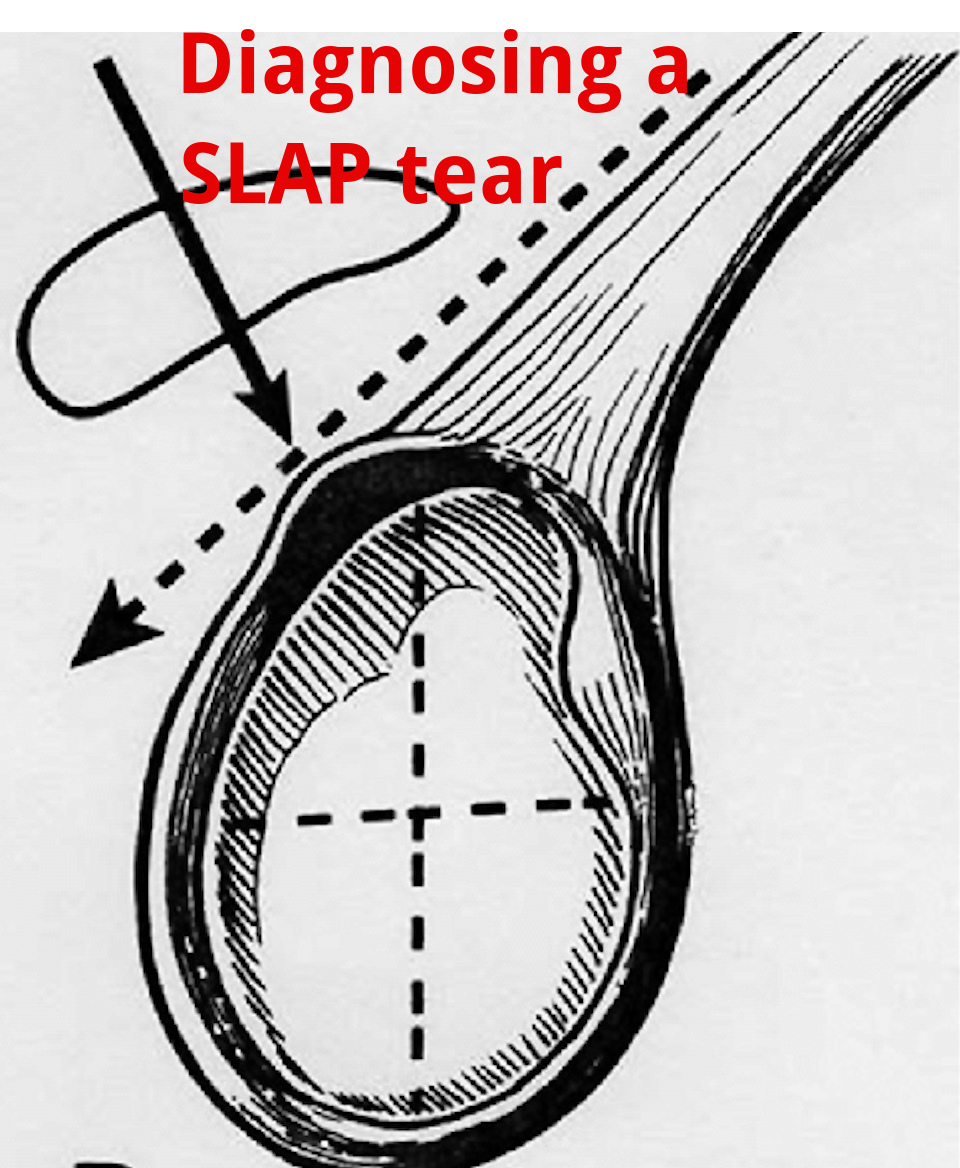
An Update on Diagnosing SLAP tears
—
by
Diagnosing a SLAP tear is not easy We hear a lot about trying to diagnose shoulder pain and to be as specific as possible. It’s often difficult to differentiate SLAP (superior labrum anterior to posterior) tears from other soft tissue injuries of the shoulder. For a review of the different types of SLAP tears, check…
-

Is Early Physical Therapy Safe After a Rotator Cuff Repair?
—
by
Physical therapy is vital after a rotator cuff repair and continues to be common in an outpatient setting. Unfortunately, there’s no true consensus on when to actually begin PT. Is early physical therapy safe after a rotator cuff repair or should we delay PT to protect the healing tendons? Let’s dive into this and see what the research…
-

Treating Patients with Low Back Pain
My thoughts on treating low back pain As many of you may know, I have been practicing physical therapy since 2003. Throughout that time, the clear majority of my patients have had injuries to their extremities. Yet, I somehow was able to ‘avoid’ treating patients with low back pain (LBP). As has been with most…