Category: knee
-

What Actually Changes After ACL Surgery
We recently had a staff meeting and were discussing our ACL Vald metric data and how we interpret it for our patients. As you know, there’s a ton of research on ACL rehab, but not a lot that actually tells you what’s happening week to week and across the full first year in the same…
-
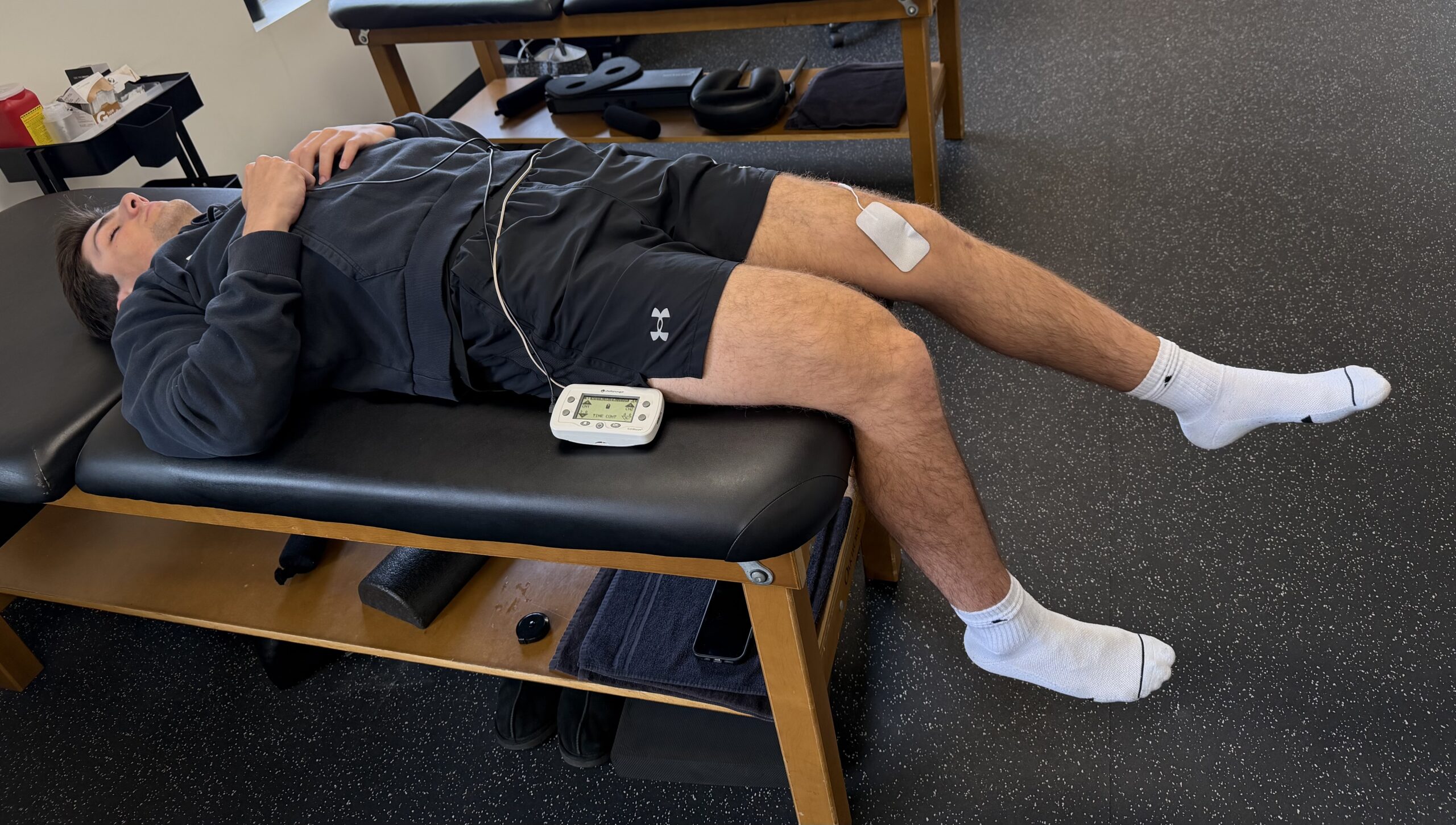
Why Your Quad Tendon ACL Patient’s Quad Is Lagging
By Lenny Macrina, MSPT, CSCS I’ve been publicly skeptical of the quad tendon (QT) graft for ACL reconstruction for a while now. If you follow me on social media, you’ve probably seen me lean toward the patellar tendon as my preferred graft, partly because of the outcomes data, partly because of what I see clinically…
-

Meniscus Repair Rehab: What Does the Evidence Actually Say?
By Lenny Macrina, MSPT, CSCS | Champion PT & Performance I get asked about meniscus repair rehab all the time. And honestly? It’s one of the most variable, most debated areas in sports PT right now (besides ACL graft choices haha). Depending on which surgeon you’re working with, you might see wildly different protocols —…
-
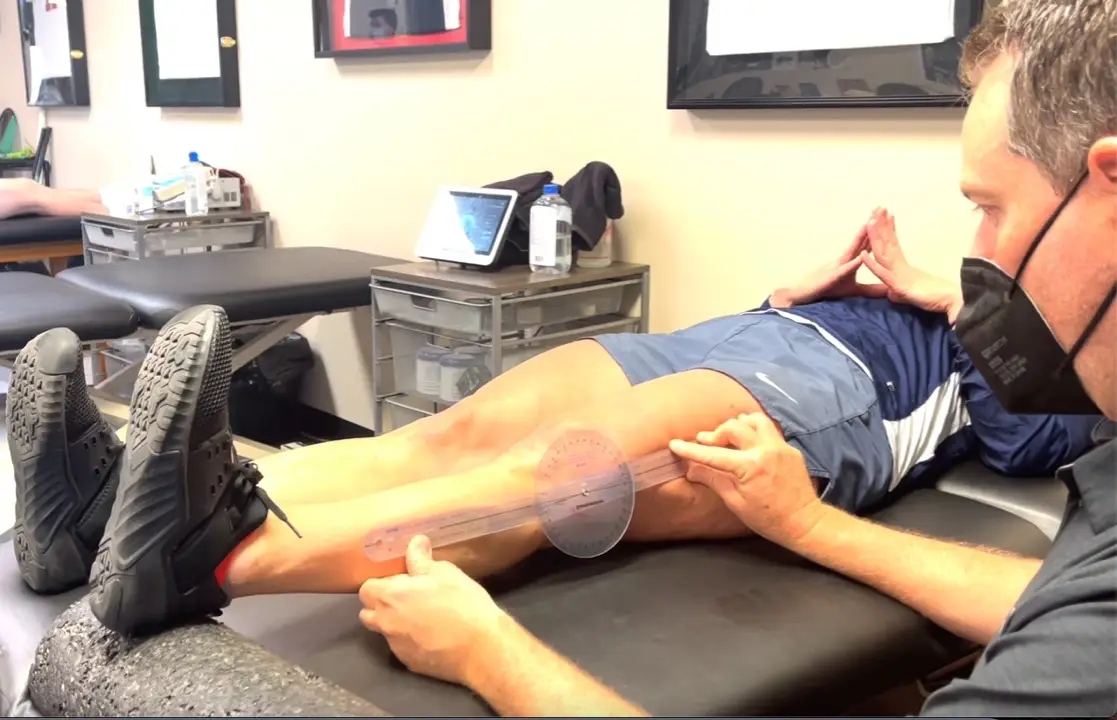
Simplifying ACL Rehab
—
by
ACL surgery continues to be a huge focus in the literature and in our outpatient rehabilitation settings. Numerous studies focus on return to play guidelines and retear rates. Social media is all over the place, most times. Let’s try to make things simple and set the stage early. Paralysis by Analysis- What ACL tests are…
-
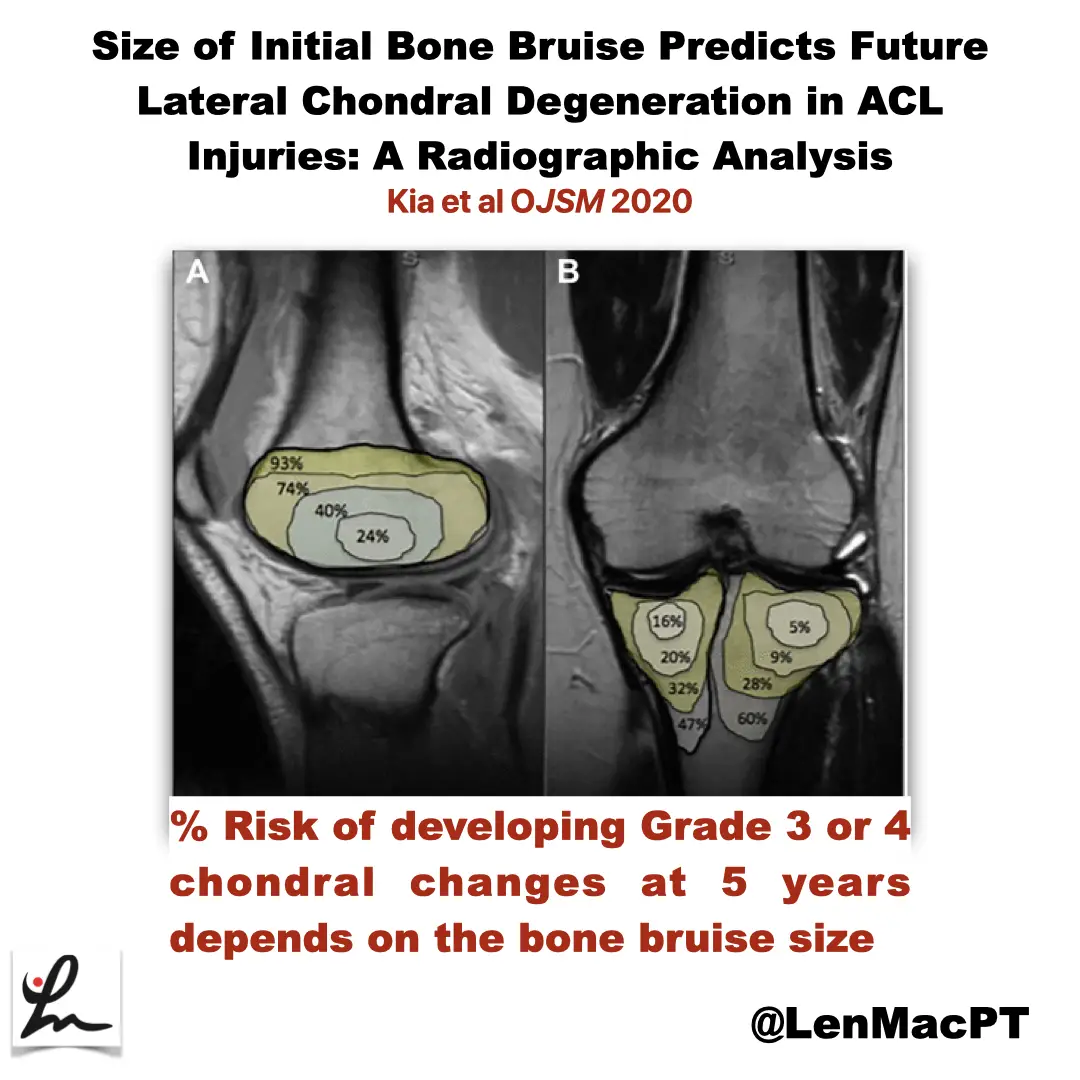
ACL tears and bone bruises
—
by
Research Review Not sure if you saw my recent post on social media about bone bruises after an ACL tear so I wanted to discuss it further here. In this study, the authors looked at the incidence of radiographic chondral changes (without correlation with clinical and functional outcomes) on MRI 5 years after the ACL…
-

ACL Volume Changes over a Women’s Soccer Season
I’m a bit interested, confused and looking to seek more on this open access paper that just came out in March of 2019 looking at the effects of season-long participation on ACL volume in female intercollegiate soccer athletes. The title of the paper is: “Effects of season-long participation on ACL volume in female intercollegiate soccer…
-
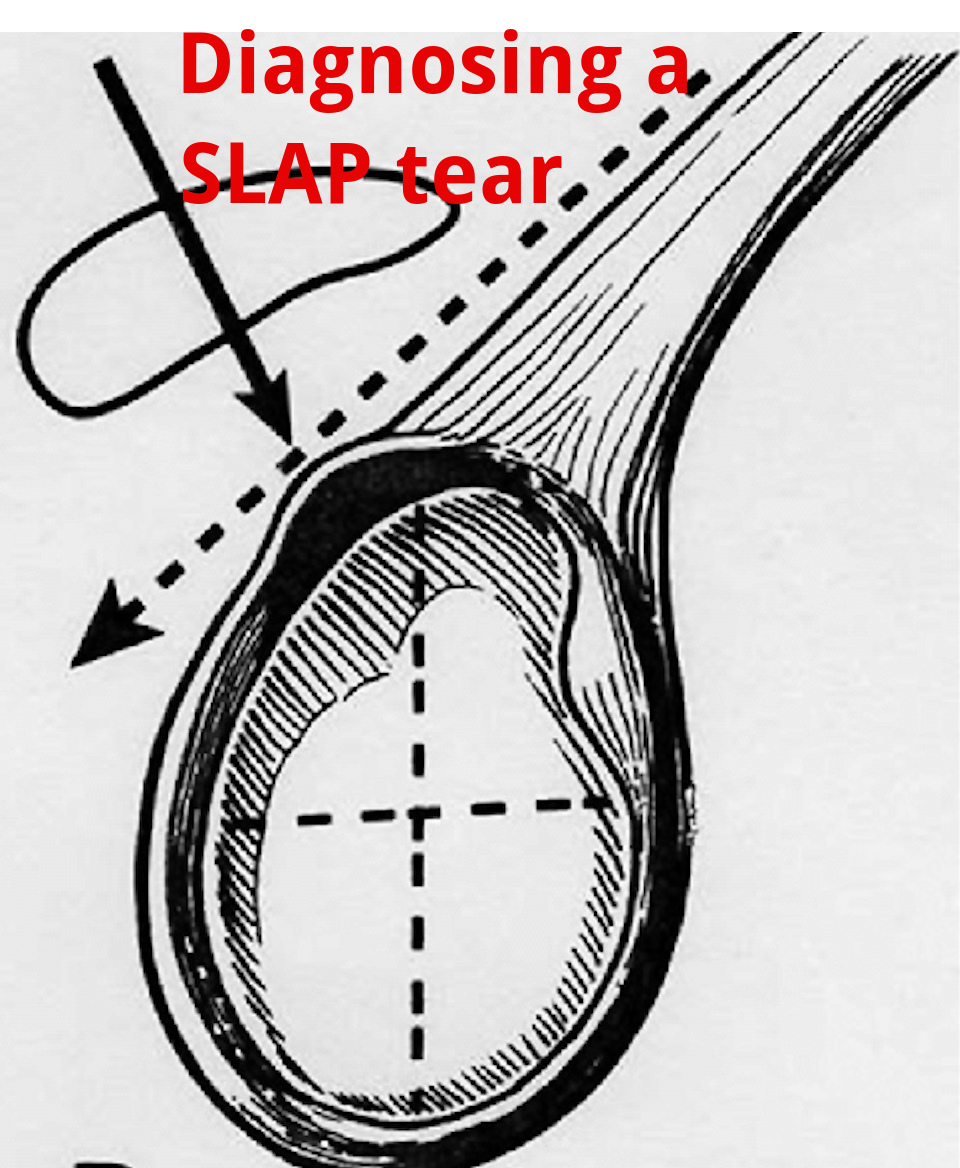
An Update on Diagnosing SLAP tears
—
by
Diagnosing a SLAP tear is not easy We hear a lot about trying to diagnose shoulder pain and to be as specific as possible. It’s often difficult to differentiate SLAP (superior labrum anterior to posterior) tears from other soft tissue injuries of the shoulder. For a review of the different types of SLAP tears, check…
-

Why you need “Feel” as a Physical Therapist
Just thinking…some recent observations of first hand experiences from the field of physical therapy.
-

The Week in Research Review, etc 12-24-18
The Week in Research Review, etc 12-24-18 only had two posts to social media this week but hopefully two very helpful posts for your practice. The back pain post was a repost from a previous time but I thought it was very important to share it again. I also put a new post from my…
-

The Week in Research Review, etc 12-17-18
—
by
Not a lot this week…sorry folks. Focusing a bit more on other projects. The Week in Research Review, etc 12-10-18 included only 3 posts but they definitely made some waves. Especially my latest Instagram post on burn-out in the PT field. Check it out and chime in…it’s never too late to like a post and comment…