By Lenny Macrina, MSPT, CSCS
I’ve been publicly skeptical of the quad tendon (QT) graft for ACL reconstruction for a while now. If you follow me on social media, you’ve probably seen me lean toward the patellar tendon as my preferred graft, partly because of the outcomes data, partly because of what I see clinically coming through our doors at Champion PT & Performance.
QT graft usage is growing. More and more surgeons are using it, especially for revision cases. And the surgical literature is actually pretty favorable. That means more QT patients are landing in your clinic, and whether you like the graft or not, these patients deserve the best possible rehab.
So I’ve been doing a deep dive on the literature and I want to share what I’ve learned, including something that I think a lot of rehab clinicians are completely missing when it comes to why quad recovery after QT tends to lag behind patellar and even hamstring grafts.
First, Why Does the Quad Come Back Slower?
If you’ve rehabbed a lot of these patients, you already know the frustration. You’re doing everything right:
✅ Early quad activation,
✅ NMES,
✅ Progressive OKC,
✅ CKC loading,
and yet the quad strength numbers just don’t climb the way they do after a patellar tendon graft. Your patient is doing the work, but the muscle isn’t responding the way you’d expect.
There are a few reasons for this.
The QT graft is harvested directly from the extensor mechanism, specifically from the superficial layer of the tendon, which comes from rectus femoris. Unlike a patellar tendon harvest, where the donor site is below the patella and somewhat separate from the primary quad muscle belly, the QT harvest site is intimately connected to the quad musculature itself. Every time you aggressively load the quad early, you’re also tensioning the exact tissue that was just cut.
On top of that, the QT consists of three distinct layers, a superficial layer from rectus femoris, an intermediate layer from vastus medialis and vastus lateralis, and a deep layer from vastus intermedius. The graft typically comes from that superficial rectus femoris layer, which means you have a unique opportunity to target that specific structure in your rehab prescription.
Add arthrogenic muscle inhibition (AMI) on top of donor-site disruption, and you’ve got a patient whose quad is fighting and beat down.
What the Delaware Group Has Been Saying
Most of you know Lynn Snyder-Mackler’s work out of the University of Delaware. Her group has set the standard for ACL rehab for decades, criterion-based milestones, aggressive early quad work, NMES, the ACL-SPORTS trial. Good stuff.
Their 2022 updated guideline in Sports Health (Brinlee, Dickenson, Hunter-Giordano, Snyder-Mackler) is worth reading in full if you haven’t. They explicitly call out that graft type should influence your rehab decisions, and they were ahead of the curve in saying that OKC knee extensions, including from day one post-op, is not just safe, but necessary. ROM modification for OKC should be driven by graft-site pain and patellofemoral stress, not by theoretical ACL strain concerns.
They also validated what a lot of us already knew: BPTB patients take longer to hit quad strength milestones and RTS criteria than hamstring or allograft patients (Smith, Capin, Zarzycki, Snyder-Mackler, JOSPT 2020). Given that QT and BPTB are both quad-harvested grafts, expect a similar or even longer timeline with QT. Your patient isn’t failing, they just need a longer runway and more time!
And if you’re not using NMES with these patients, start. The 2024 paper from the same group (Arhos, Ito, Hunter-Giordano, Nolan, Snyder-Mackler, Silbernagel, JOSPT) is a good clinical refresher. It lays out exactly why most clinicians either aren’t using it or aren’t dosing it therapeutically. High-intensity NMES from the start is the standard, not an optional add-on.
I use Chattanooga’s Continuum2 and try to get the muscle activated as much as possible but replicating the Delaware protocol is difficult at times. Do your best and try to increase the NMES intensity within each session to maximize muscle output.
The Hip Position And Why It Actually Matters for QT Grafts
Here’s where I want to spend some time, because this is the piece that most people are missing, and it’s a genuinely QT specific modification that doesn’t apply the same way to patellar or hamstring graft rehab.
A 2023 clinical commentary in IJSPT by Solie, Monson, and Larson makes a recommendation that sounds simple but has real biomechanical logic behind it:
When your QT patient does OKC knee extension, consider positioning them in supine (hip neutral or extended) rather than the typical seated position at 80–90° of hip flexion.
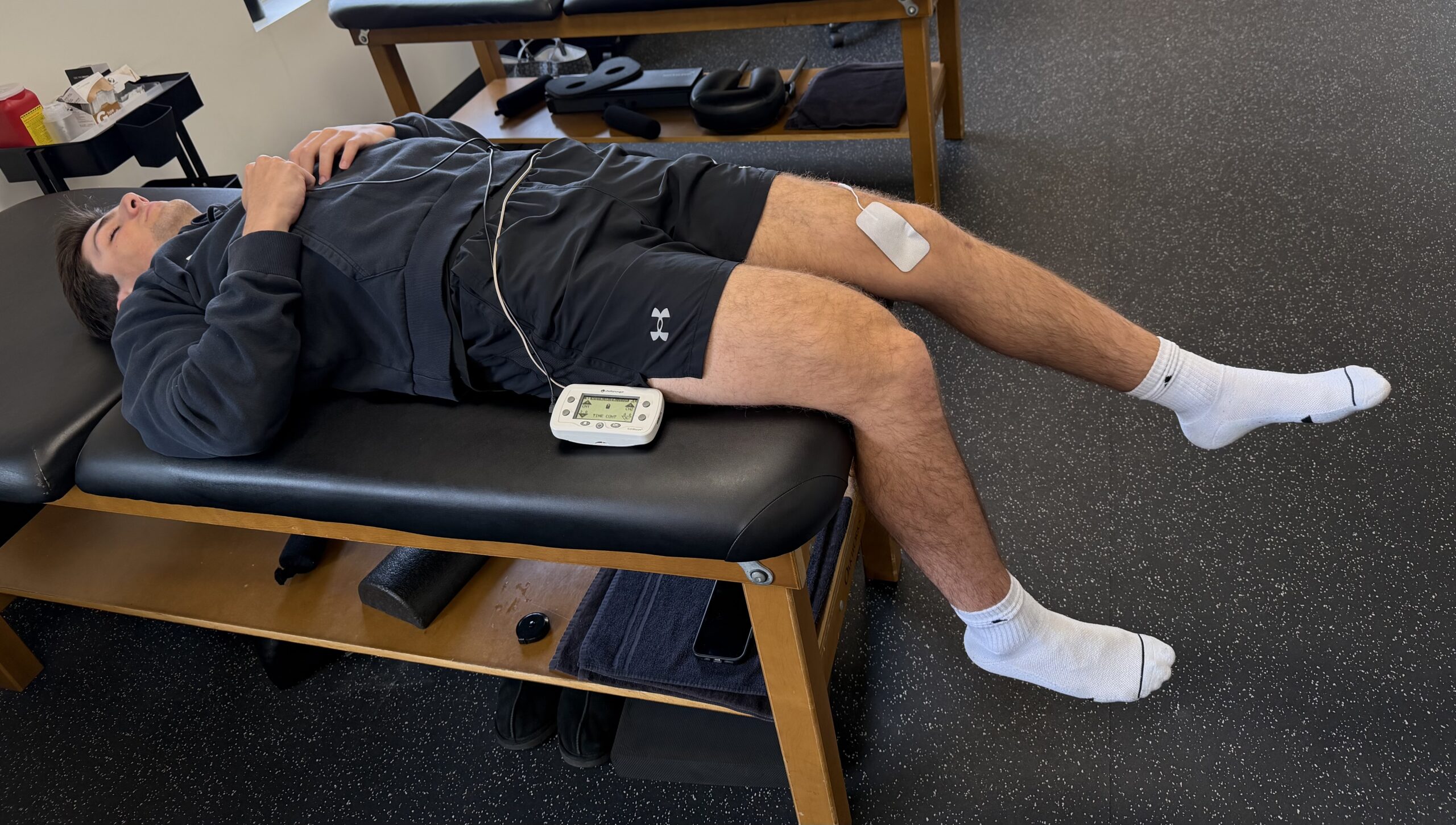
The research shows that seated knee extension produces about 8% more peak torque than supine knee extension, and greater muscle swelling in the vastus lateralis. If the goal is maximal quad output, why would you take the patient out of the position that generates more force?
The answer is that for a QT patient, the goal isn’t just maximal quad torque, it’s targeted loading of rectus femoris, which is the exact layer that was harvested.
Rectus femoris is a biarticular muscle. It crosses both the hip and the knee. When you’re seated (hip flexed at ~85–90°), the rectus femoris is shortened at the hip, which puts it at a relative mechanical disadvantage for contributing to force production, but it also means it’s somewhat unloaded. When you’re supine (hip at or near 0°), the rectus femoris is lengthened at the hip, which puts it under more tension and preferentially loads it during knee extension.
So supine OKC isn’t a weaker position, it’s the position that makes rectus femoris work harder. For a QT patient, that’s what you want early in rehab. By using targeted and deliberate progressive loading, particularly of the QT, this could aid in graft-site tissue healing, without the volume or intensity that would cause irritability.
The “Oh My Quad” paper in IJSPT (2025) also adds some useful insight here. Training at longer muscle lengths drives better hypertrophic adaptations than training at shortened lengths. For rectus femoris in a QT patient, supine positioning achieves exactly that!
How I’m Thinking About This Clinically
Here’s how I’d conceptualize the progression for a QT patient:
Early phase (0–6 weeks): Supine or reclined OKC active range of motion first, then light resistance progressed by graft-site pain and effusion response, not by time. NMES at high intensity or as tolerated from day one, knee at 60° of flexion for the stimulation setup. Full ROM OKC is safe and appropriate; don’t let fear of graft strain push you toward excessive restriction but I wouldn’t load it heavy just yet. Even consider Blood Flow Restriction (BFR) in this phase to help with muscle hypertrophy.
Mid phase (6–16 weeks): Transition toward a more seated position as graft-site irritability decreases and you want to shift loading deeper into the QT toward the vastus layers. CKC loading should move from isometric at low knee flexion angles to isotonic with progressive resistance. The seated leg extension machine earns its place here.
Important caution in later phases: The combined position of hip extension AND knee flexion under load is where the QT graft sees maximum stress, sorta like the wind-up phase of kicking, or the swing phase of high-velocity running. Sagittal plane deceleration is another big one. These need to be progressed carefully and monitored for graft-site irritability, even after strength milestones are met.
What I Got Wrong And What This Changes for Me
I’ve been so focused on outcomes data comparing graft types that I undervalued the graft-specific rehab piece. The honest truth is that a lot of the “QT takes forever to recover” frustration in the clinic may not be a graft failure, it may just be a rehab modification away. We’ve been applying BPTB or hamstring rehab logic to a graft that behaves differently, targets a different donor site, and needs a different loading strategy.
That doesn’t mean I’m suddenly in love with the QT graft for every patient, trust me! But it does mean that if your surgeon is using it, you owe it to your patient to understand the nuance.
The literature here is still catching up. There’s no large RCT comparing graft-specific rehab protocols for QT versus the alternatives. The Solie et al. commentary is Level 5 evidence, expert opinion based on anatomy and biomechanical reasoning. We need better data. But in the meantime, the logic is sound, and clinically it’s not a high-risk modification to implement.
I’m still trying to understand how to best rehab a patient’s ACL surgery after a QT graft and I hope this post sheds some light. Please share it with your friends and coworkers and let’s better understand this rehab as a group.
Instead of getting frustrated DM’s from patients and clinicians, I’m hoping to change the narrative and get more positive outcomes and tips to help our patients get strong faster, and back to the sports they love!
Summary for Busy Clinicians
- QT patients struggle with quad recovery partly because the graft comes from the superficial rectus femoris layer, directly disrupting the extensor mechanism in a way HS and BPTB grafts don’t.
- Early OKC is safe and necessary, don’t delay it out of graft strain fear; modify ROM based on graft-site pain and PF stress instead.
- Consider supine OKC in early rehab to preferentially load rectus femoris and the harvest site, not because it produces more overall torque, but because it targets the right structure.
- Transition toward seated OKC as rehabilitation progresses to shift loading to the deeper vastus layers.
- Use high-intensity NMES from the start, it’s an “A” grade recommendation and still dramatically underutilized.
- Late-stage caution: hip extension + knee flexion under load is the maximum stress position for the QT; progress deceleration, kicking mechanics, and high-velocity running accordingly.
Key References
- Brinlee AW, Dickenson SB, Hunter-Giordano A, Snyder-Mackler L. ACL reconstruction rehabilitation: clinical data, biologic healing, and criterion-based milestones to inform a return-to-sport guideline. Sports Health. 2022;14(5):770-779.
- Smith AH, Capin JJ, Zarzycki R, Snyder-Mackler L. Athletes with BPTB autograft for ACLR were slower to meet rehabilitation milestones and RTS criteria than athletes with HS autograft or soft tissue allograft. J Orthop Sports Phys Ther. 2020;50(5):259-266.
- Solie B, Monson J, Larson C. Graft-specific surgical and rehabilitation considerations for ACLR with the quadriceps tendon autograft. Int J Sports Phys Ther. 2023;18(2):493-512.
- Arhos EK, Ito N, Hunter-Giordano A, Nolan TP, Snyder-Mackler L, Silbernagel KG. Who’s afraid of electrical stimulation? Let’s revisit the application of NMES at the knee. J Orthop Sports Phys Ther. 2024;54(2):101-106.
- Noehren B, Snyder-Mackler L. Who’s afraid of the big bad wolf? Open-chain exercises after anterior cruciate ligament reconstruction. J Orthop Sports Phys Ther. 2020;50(9):473-475.
- Hunnicutt JL, Slone HS, Xerogeanes JW. Implications for early postoperative care after quadriceps tendon autograft for ACLR: a technical note. J Athl Train. 2020;55:623-627.
Questions or feedback? Find me on Instagram @lenmacpt or X @lenmacpt
Leave a Reply