Tag: physical therapy
-

What Actually Changes After ACL Surgery
We recently had a staff meeting and were discussing our ACL Vald metric data and how we interpret it for our patients. As you know, there’s a ton of research on ACL rehab, but not a lot that actually tells you what’s happening week to week and across the full first year in the same…
-
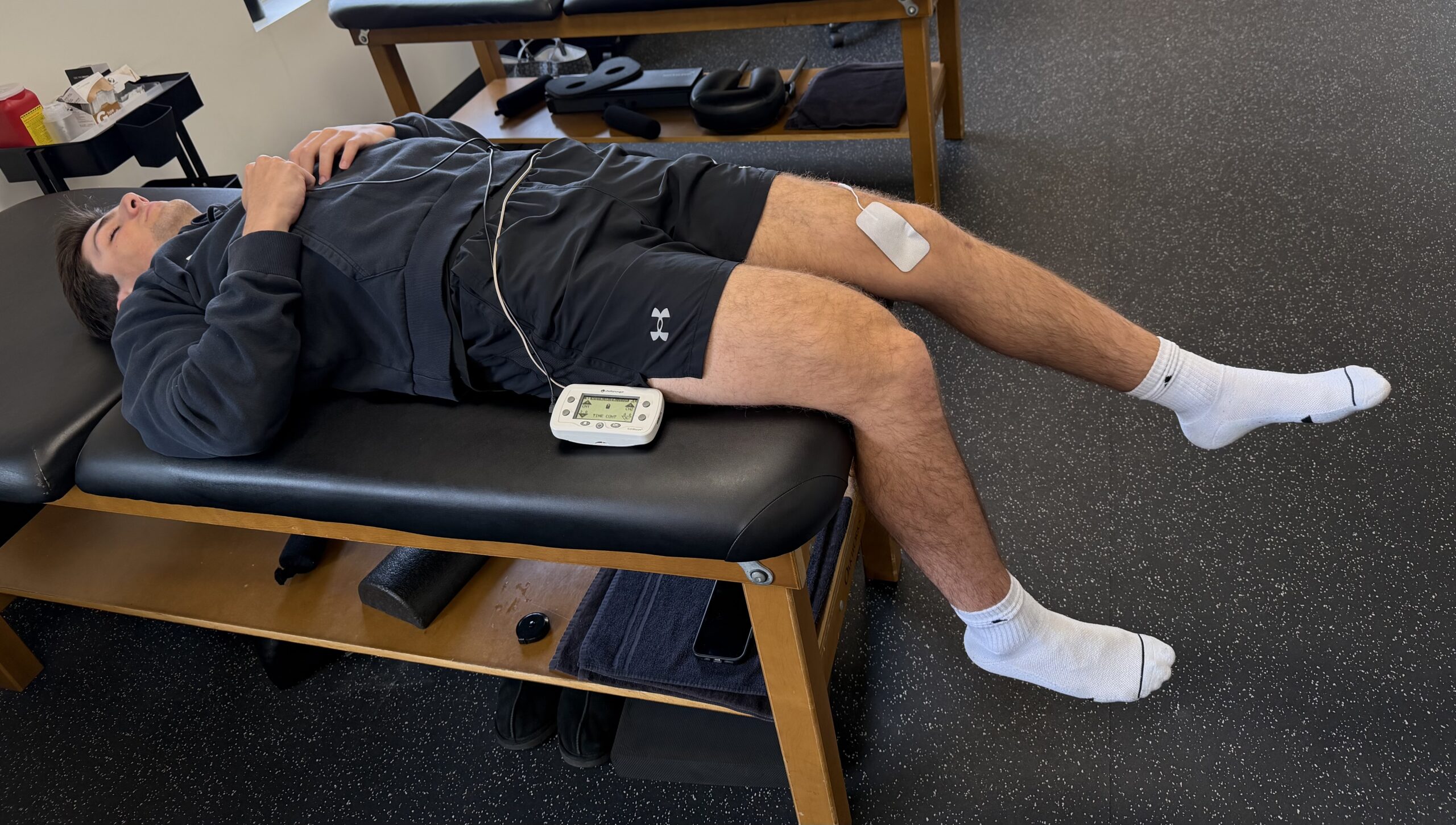
Why Your Quad Tendon ACL Patient’s Quad Is Lagging
By Lenny Macrina, MSPT, CSCS I’ve been publicly skeptical of the quad tendon (QT) graft for ACL reconstruction for a while now. If you follow me on social media, you’ve probably seen me lean toward the patellar tendon as my preferred graft, partly because of the outcomes data, partly because of what I see clinically…
-

Meniscus Repair Rehab: What Does the Evidence Actually Say?
By Lenny Macrina, MSPT, CSCS | Champion PT & Performance I get asked about meniscus repair rehab all the time. And honestly? It’s one of the most variable, most debated areas in sports PT right now (besides ACL graft choices haha). Depending on which surgeon you’re working with, you might see wildly different protocols —…
-

Is Early Physical Therapy Safe After a Rotator Cuff Repair?
—
by
Physical therapy is vital after a rotator cuff repair and continues to be common in an outpatient setting. Unfortunately, there’s no true consensus on when to actually begin PT. Is early physical therapy safe after a rotator cuff repair or should we delay PT to protect the healing tendons? Let’s dive into this and see what the research…
-

Treating Patients with Low Back Pain
My thoughts on treating low back pain As many of you may know, I have been practicing physical therapy since 2003. Throughout that time, the clear majority of my patients have had injuries to their extremities. Yet, I somehow was able to ‘avoid’ treating patients with low back pain (LBP). As has been with most…
-

Why you need “Feel” as a Physical Therapist
Just thinking…some recent observations of first hand experiences from the field of physical therapy.
-

The Week in Research Review, etc 12-24-18
The Week in Research Review, etc 12-24-18 only had two posts to social media this week but hopefully two very helpful posts for your practice. The back pain post was a repost from a previous time but I thought it was very important to share it again. I also put a new post from my…
-

The Week in Research Review, etc 12-17-18
—
by
Not a lot this week…sorry folks. Focusing a bit more on other projects. The Week in Research Review, etc 12-10-18 included only 3 posts but they definitely made some waves. Especially my latest Instagram post on burn-out in the PT field. Check it out and chime in…it’s never too late to like a post and comment…
-
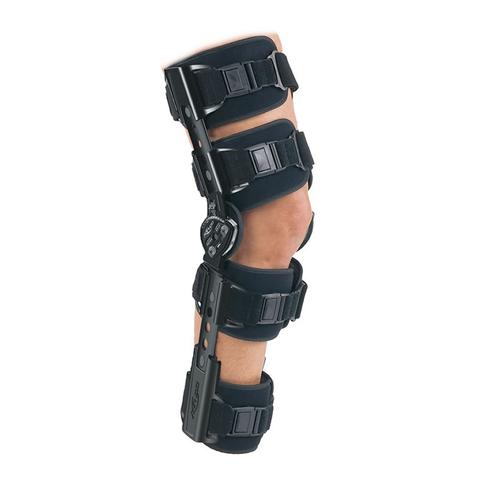
Knee Bracing Immediately After an ACL Reconstruction
I recently came across a Facebook post that discussed bracing immediately after an ACL reconstruction and I was intrigued. I read some of the comments and chimed in with my observations and opinions. In turn, a multi-platform discussion revealed many new details. I wanted to briefly share some of the research and the discussions that…
-

The Week in Research Review, etc 12-3-18
—
by
Hey everyone, The Week in Research Review, etc for this week has a new look, compliments of Instagram’s new algorithm. Hope the new format doesn’t throw you too big of a curveball (maybe you’ll like it better), so here goes… ACL Injury Rates Higher on Synthetic Turf than Natural Grass in the NFL Preventing…