Tag: physical therapist
-

The Week in Research Review, etc 10-8-18
—
by
in ACL, baseball, DPTstudent, elbow, general, hip, knee, Physical Therapy, rehabilitation, Research, rotator cuff, ShoulderHey all, the Week in Research Review, etc 10-8-18 has some great articles that really got some good discussion going. I highly recommend reading each post and chiming in. Looking forward to the new comments and discussions! PT Continuity of care Fatigue effects on ACL tears Measuring IR in a baseball pitcher Lever sign to…
-
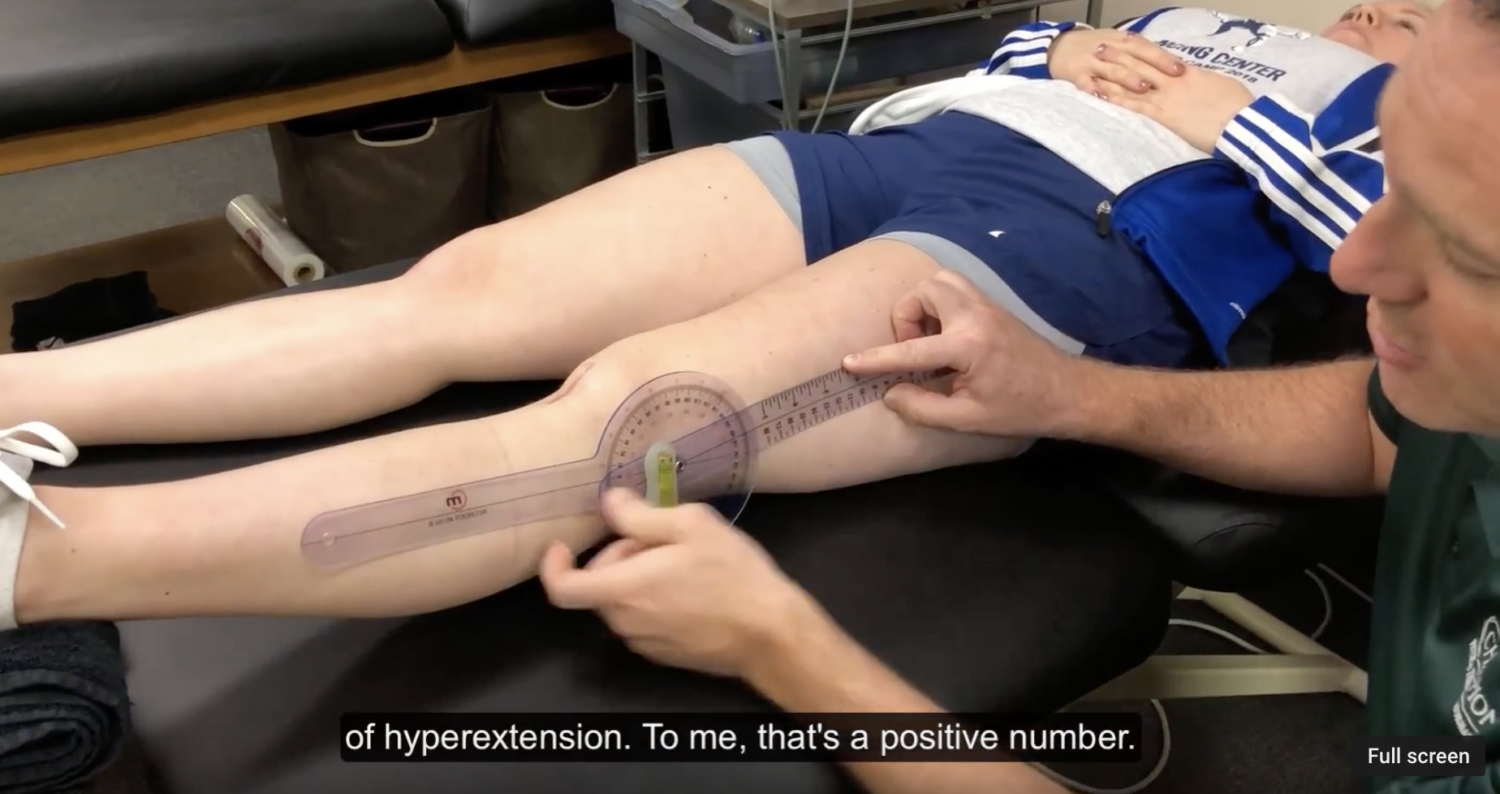
Documenting Knee Extension Range of Motion
I’ve talked a lot about the importance of regaining knee extension range of motion (ROM) after a knee injury or surgery. In this post, I want to talk about how exactly I believe we should be documenting knee extension range of motion. I think it’s important because I hear many other medical professionals and students document differently.…
-

The Week in Research Review, etc 7-22-18
—
by
The Week in Research Review, etc 7-22-18 I’m trying out this new concept of publishing my social media posts into a nice package for a weekly delivery to my subscribers. Knee Case Study Contralateral ACL Strengthening Shoulder Static Stabilizers Weighted Ball Research Glute Activation This kid came to me the other day with L knee…
