Tag: knee pain
-

The Week in Research Review, etc 11-5-18
—
by
in ACL, DPTstudent, emg, exercise, general, hip, knee, Physical Therapy, rehabilitation, Research, rotator cuff, ShoulderThe Week in Research Review, etc 11-5-18 was filled with more informative and eye-opening posts! Lots of visually stimulating posts to help clarify what exactly is going on in the hip joint with PROM. Another post that shows the suction effect from an intact hip labrum… amongst other great posts. Just some great stuff..hope you…
-

The Week in Research Review, etc 10-29-18
—
by
This week we started the week off with a couple shoulder posts, specifically the rotator cuff and SLAP tears. As usual, I can’t resist a good ACL paper so included that NM control program that should be in all knee patients’ programs. We ended the week with a recorded knee scope as the surgeon was…
-

The Week in Research Review, etc 10-22-18
—
by
That was a milestone week as my Instagram account finally hit 10k followers, whatever that means! I’ve really been pushing a daily post to help other rehab professionals better simplify the research. One milestone hit but I still want to keep publishing good quality research reviews. The Week in Research Review, etc 10-22-18 included: Do baseball Pitchers…
-

The Week in Research Review, etc 10-15-18
—
by
in ACL, baseball, DPTstudent, elbow, exercise, hip, knee, Physical Therapy, rehabilitation, Research, rotator cuff, ShoulderThis week I posted a lot of research and thoughts on shoulder and knee rehab, particularly after an ACL injury. I also shared some others posts that really complimented my posts so there’s some bonus reading to do too. Hope The Physical Therapy Week in Research Review helps your Monday patients and beyond! Take a read and…
-

The Week in Research Review, etc 10-8-18
—
by
in ACL, baseball, DPTstudent, elbow, general, hip, knee, Physical Therapy, rehabilitation, Research, rotator cuff, ShoulderHey all, the Week in Research Review, etc 10-8-18 has some great articles that really got some good discussion going. I highly recommend reading each post and chiming in. Looking forward to the new comments and discussions! PT Continuity of care Fatigue effects on ACL tears Measuring IR in a baseball pitcher Lever sign to…
-

The Week in Research Review, etc 10-1-18
—
by
Another week of some great discussions and learning opportunities. The Week in Research Review included: Risk Factors for Patellofemoral pain Shoulder ROM and elbow injuries Rotator Cuff Exercises Eccentric or Concentric exercise for Tendinopathy Hamstrings Protect the ACL Stretching the Shoulder in the Overhead Athlete Share with your friends and have them subscribe to the weekly newsletter!…
-

The Week in Research Review, etc 9-10-18
—
by
Lots of good stuff this past week. We talked: Dr. Andrews knowledge bombs Frozen Shoulder video AC joint Classification Whether we should return our ACL patients at 6 months post-op Eric Cressey quote on failing rehab What I have learned about being successful as an orthopedic surgeon by Dr James Andrews Great read by my…
-
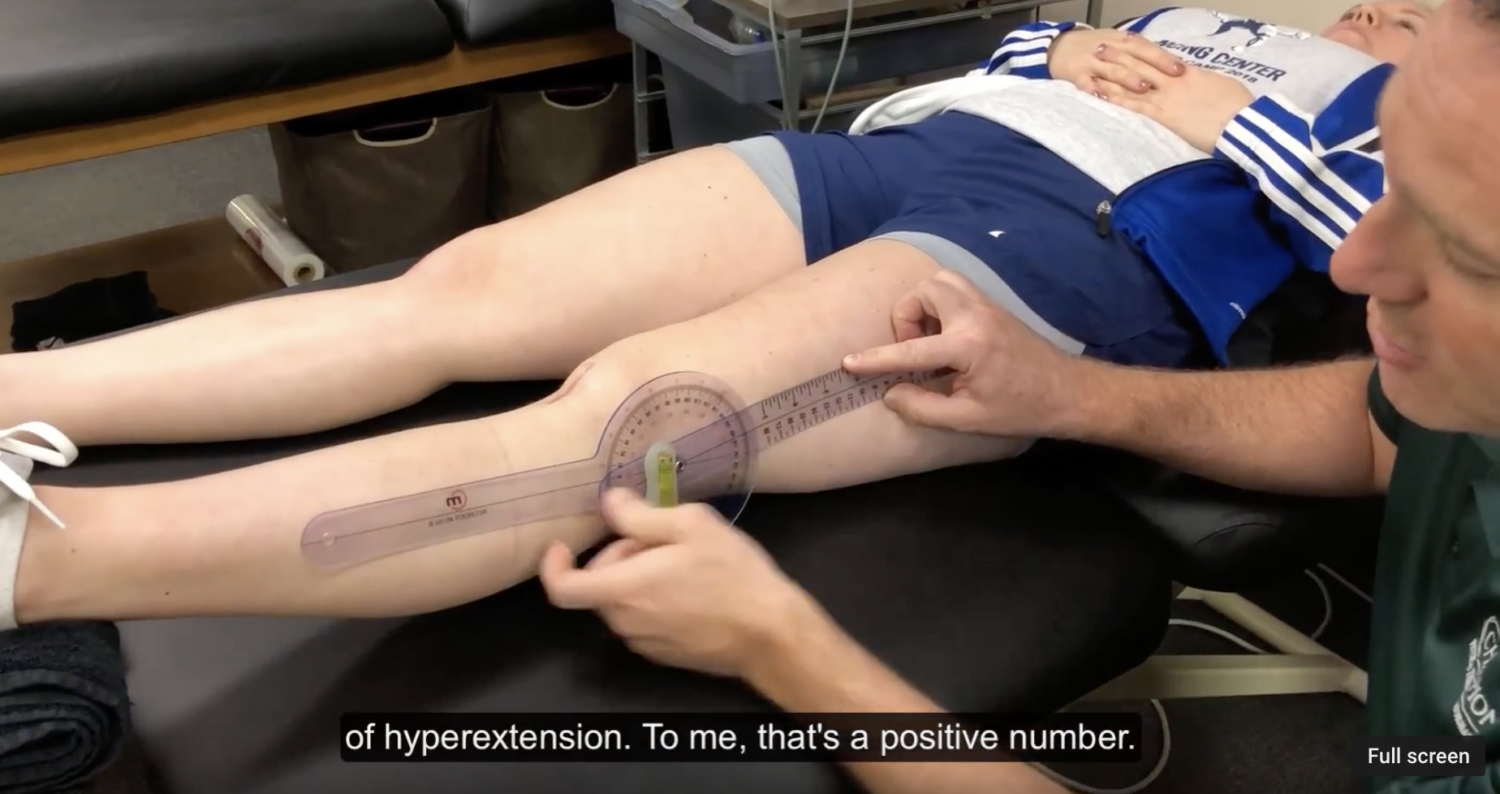
Documenting Knee Extension Range of Motion
I’ve talked a lot about the importance of regaining knee extension range of motion (ROM) after a knee injury or surgery. In this post, I want to talk about how exactly I believe we should be documenting knee extension range of motion. I think it’s important because I hear many other medical professionals and students document differently.…
-

The Week in Research Review, etc 8-5-18
—
by
The Week in Research Review, etc 8-5-18 we discuss a wide variety of topics including: Long-term disability if weak during adolescence Using heat during rehabilitation OKC vs CKC exercises after an ACL Live look at an Achilles rupture (with sound too!) A fun look at the different types of PT’s Congrats to all of the newly…
-

The Week in Research Review, etc 7-22-18
—
by
The Week in Research Review, etc 7-22-18 I’m trying out this new concept of publishing my social media posts into a nice package for a weekly delivery to my subscribers. Knee Case Study Contralateral ACL Strengthening Shoulder Static Stabilizers Weighted Ball Research Glute Activation This kid came to me the other day with L knee…