Category: elbow
-

The Week in Research Review, etc 8-5-18
—
by
The Week in Research Review, etc 8-5-18 we discuss a wide variety of topics including: Long-term disability if weak during adolescence Using heat during rehabilitation OKC vs CKC exercises after an ACL Live look at an Achilles rupture (with sound too!) A fun look at the different types of PT’s Congrats to all of the newly…
-

The Week in Research Review, etc 7-29-18
—
by
Last week was the 1st of my research review that summarized my social media posts from the previous week. It seemed to be well received so I figured I’d continue it. My goal is to help summarize some of the research that I found interesting and package it nicely for my readers. Each photo contains…
-

The Week in Research Review, etc 7-22-18
—
by
The Week in Research Review, etc 7-22-18 I’m trying out this new concept of publishing my social media posts into a nice package for a weekly delivery to my subscribers. Knee Case Study Contralateral ACL Strengthening Shoulder Static Stabilizers Weighted Ball Research Glute Activation This kid came to me the other day with L knee…
-
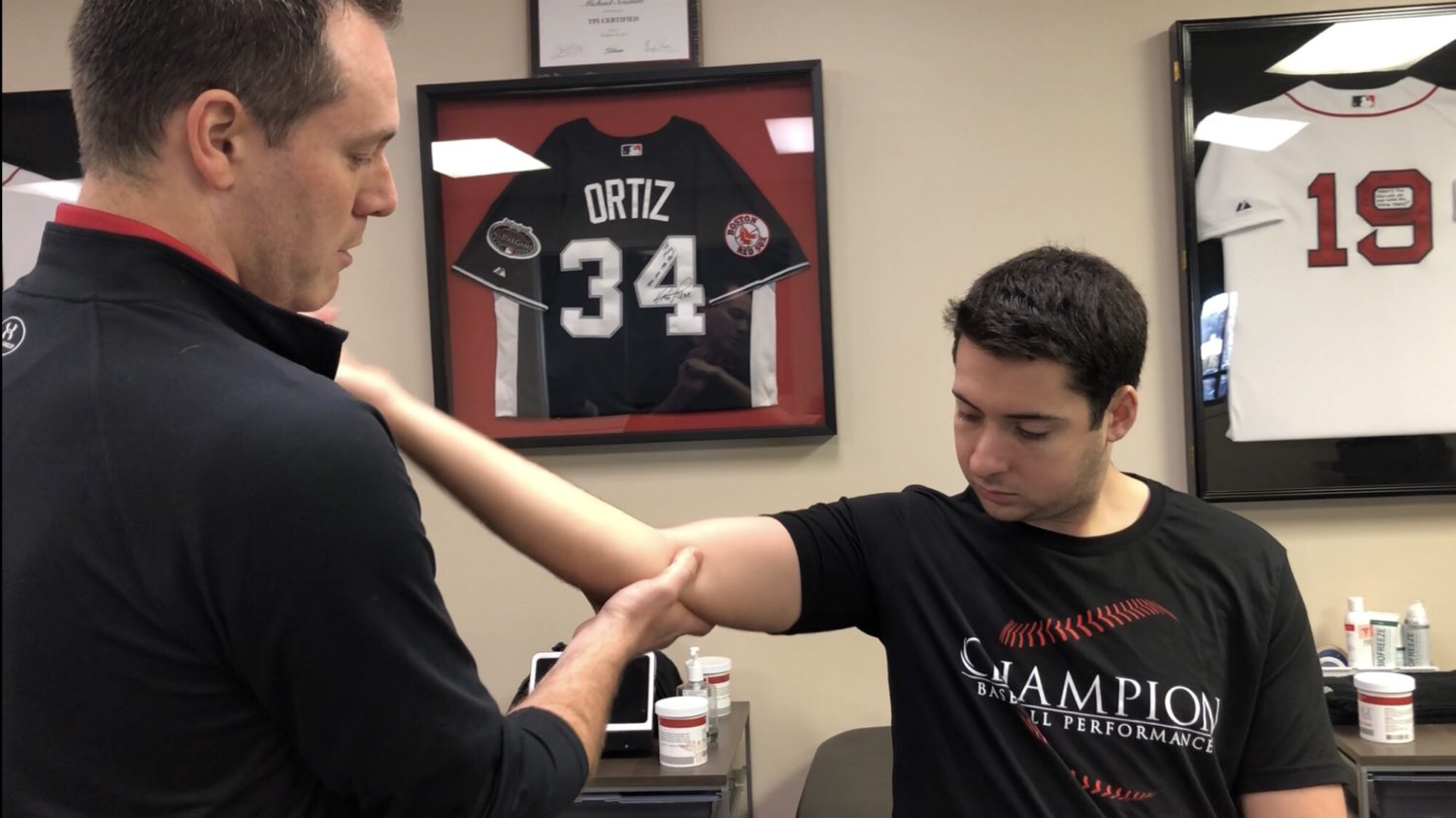
Testing the elbow for a UCL sprain in baseball players
I have assessed hundreds if not thousands of elbows for various injuries. One of the most common ailments that I see in my practice is a UCL (ulnar collateral ligament) sprain, aka ‘Tommy John ligament’, especially in a baseball player. This post discusses the typical presentation of a UCL sprain, testing the elbow for a UCL…
