Tag: physiotherapy
-

Treating Patients with Low Back Pain
My thoughts on treating low back pain As many of you may know, I have been practicing physical therapy since 2003. Throughout that time, the clear majority of my patients have had injuries to their extremities. Yet, I somehow was able to ‘avoid’ treating patients with low back pain (LBP). As has been with most…
-

The Week in Research Review, etc 12-24-18
The Week in Research Review, etc 12-24-18 only had two posts to social media this week but hopefully two very helpful posts for your practice. The back pain post was a repost from a previous time but I thought it was very important to share it again. I also put a new post from my…
-

The Week in Research Review, etc 12-17-18
—
by
Not a lot this week…sorry folks. Focusing a bit more on other projects. The Week in Research Review, etc 12-10-18 included only 3 posts but they definitely made some waves. Especially my latest Instagram post on burn-out in the PT field. Check it out and chime in…it’s never too late to like a post and comment…
-
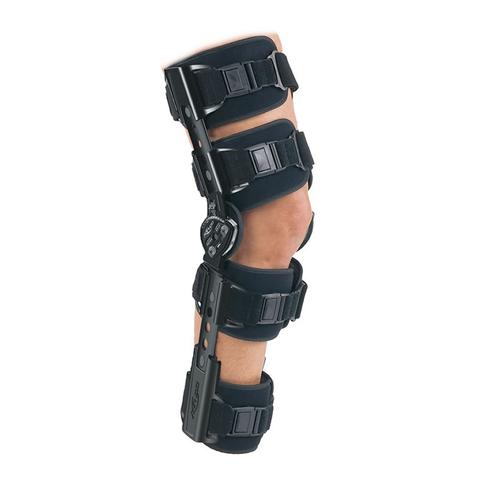
Knee Bracing Immediately After an ACL Reconstruction
I recently came across a Facebook post that discussed bracing immediately after an ACL reconstruction and I was intrigued. I read some of the comments and chimed in with my observations and opinions. In turn, a multi-platform discussion revealed many new details. I wanted to briefly share some of the research and the discussions that…
-

The Week in Research Review, etc 12-3-18
—
by
Hey everyone, The Week in Research Review, etc for this week has a new look, compliments of Instagram’s new algorithm. Hope the new format doesn’t throw you too big of a curveball (maybe you’ll like it better), so here goes… ACL Injury Rates Higher on Synthetic Turf than Natural Grass in the NFL Preventing…
-

The Week in Research Review, etc 11-26-18
This week, I discussed the progression of someone after a knee surgery. I tried to highlight the key stages and some techniques that I like to use to advance the patient’s mobility and comfort. Take a look at The Week in Research Review, etc 11-26-18 and share with your friends. Hope it helps you improve your…
-

The Week in Research Review, etc 11-19-18
—
by
Great ‘Week in Research Review, etc 11-19-18’ that I hope you find helpful to your practice. I’ve always touted the importance of the subjective portion of the exam so I wanted to share a slide from a recent talk I gave to a group in Canandaigua, NY. Obviously, the squat is a fundamental movement and…
-

The Week in Research Review, etc 11-12-18
—
by
This week in research review for 11-12-18 we focused a bit more on assessment and also dabbled in some basic treatment strategies for the back and shoulder. Check out the topics below and like them or comment on Instagram to keep the conversation going…thanks all! A quick fix for a sore low back? Knee…
-

The Week in Research Review, etc 10-29-18
—
by
This week we started the week off with a couple shoulder posts, specifically the rotator cuff and SLAP tears. As usual, I can’t resist a good ACL paper so included that NM control program that should be in all knee patients’ programs. We ended the week with a recorded knee scope as the surgeon was…
-
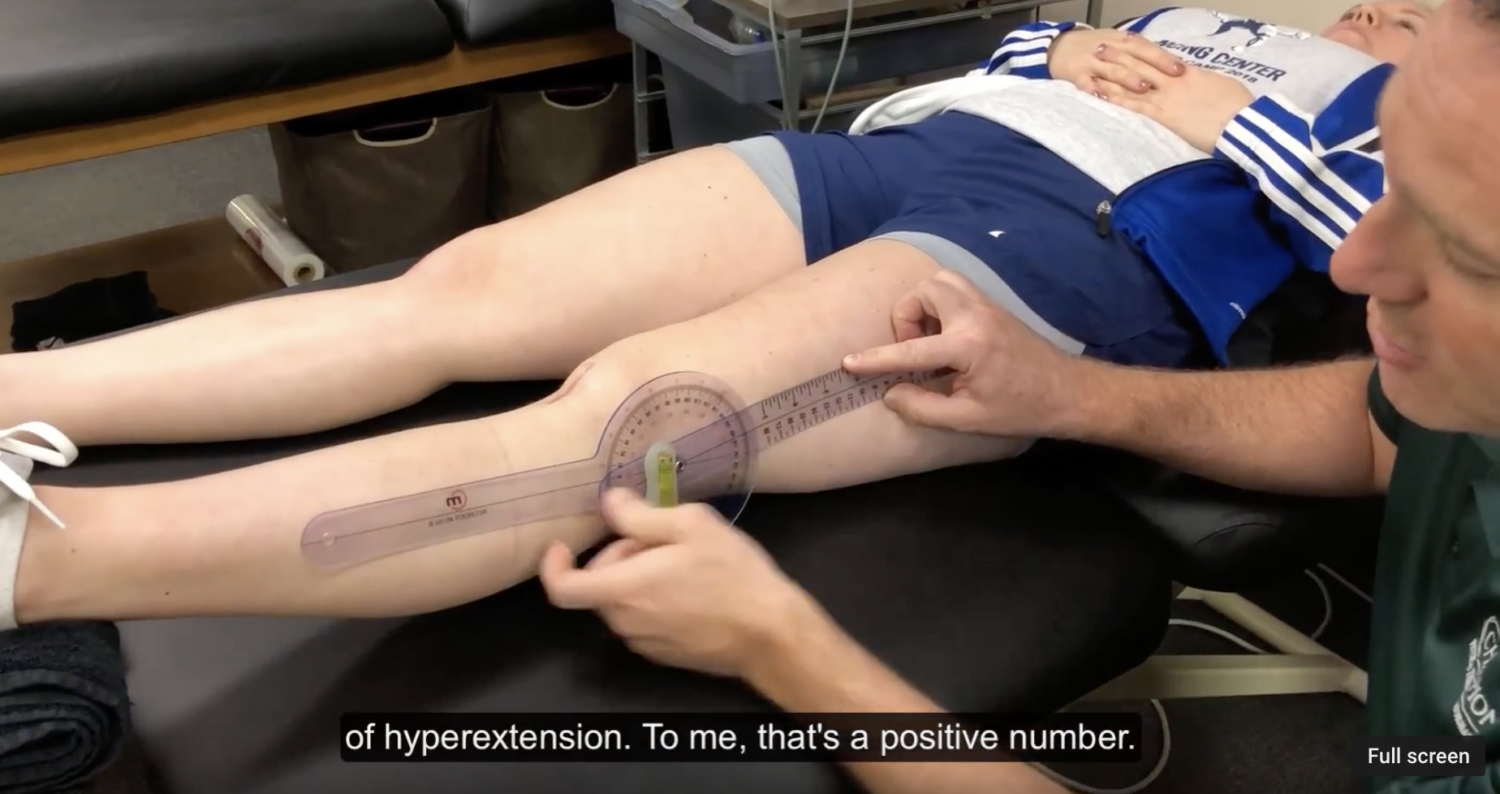
Documenting Knee Extension Range of Motion
I’ve talked a lot about the importance of regaining knee extension range of motion (ROM) after a knee injury or surgery. In this post, I want to talk about how exactly I believe we should be documenting knee extension range of motion. I think it’s important because I hear many other medical professionals and students document differently.…