Category: knee
-
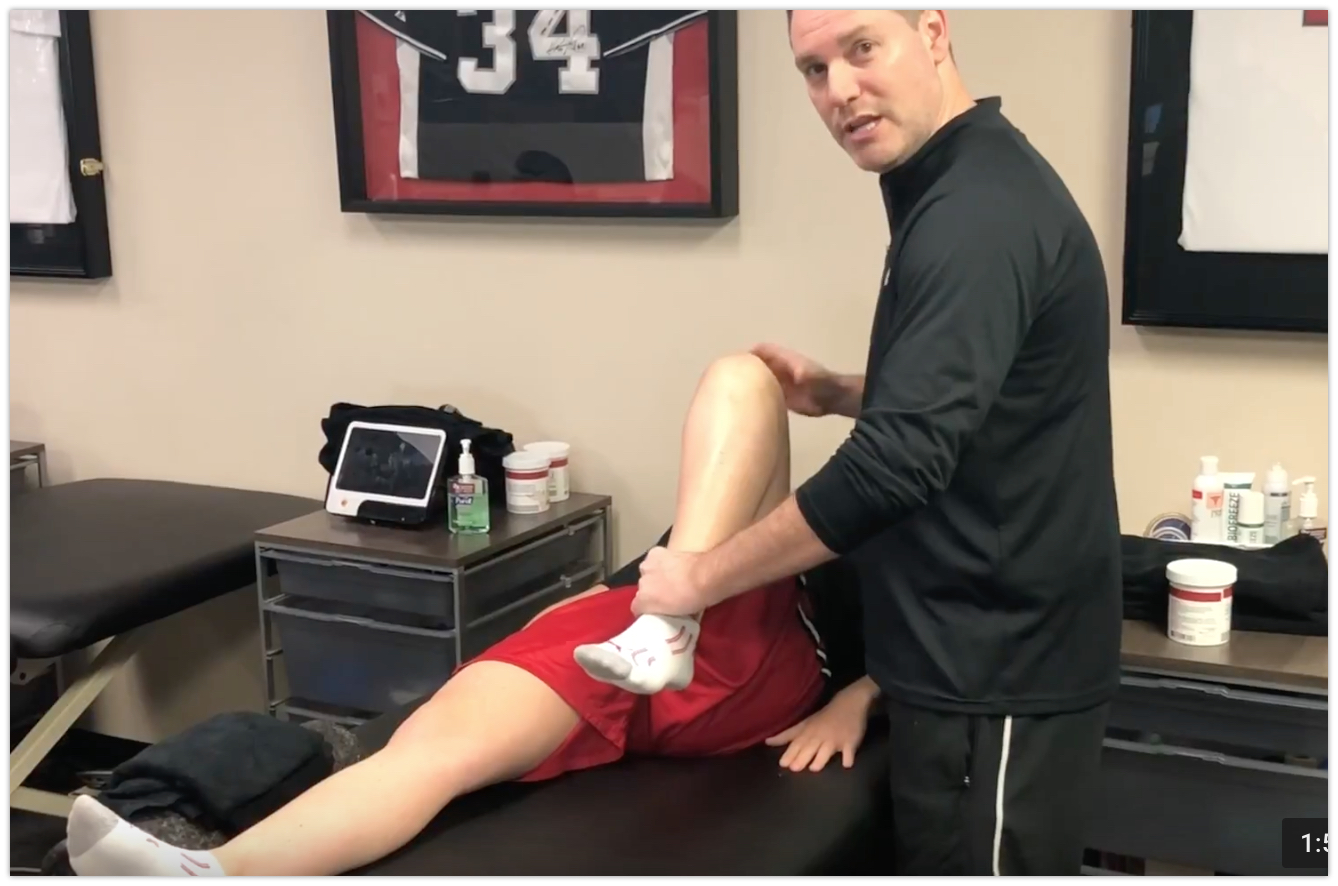
Quadriceps Stretching after Knee Surgery: A tweak to the technique
Obtaining full knee flexion after a knee surgery or knee injury can be difficult for some. The transition from passive knee flexion in seated (my preferred) or supine (not preferred!) can be a challenge for the physical therapist, once they are starting to work on quadriceps stretching. This blog post serves to help modify the…
-
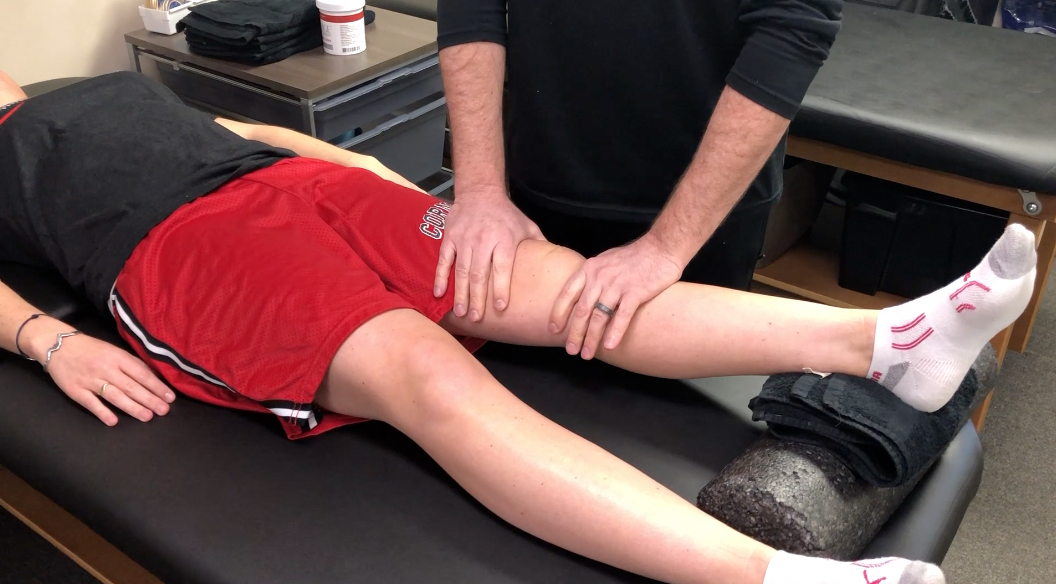
Loss of extension after ACL surgery: How to assess for a cyclops lesion
Loss of extension after an ACL reconstruction can be debilitating for the patient. It’s not as common as you would think but I see it enough in the clinic from people that are months out from surgery. Usually, this loss of knee extension after an ACL reconstruction is caused by a cyclops lesion. Let’s dive deeper…
-
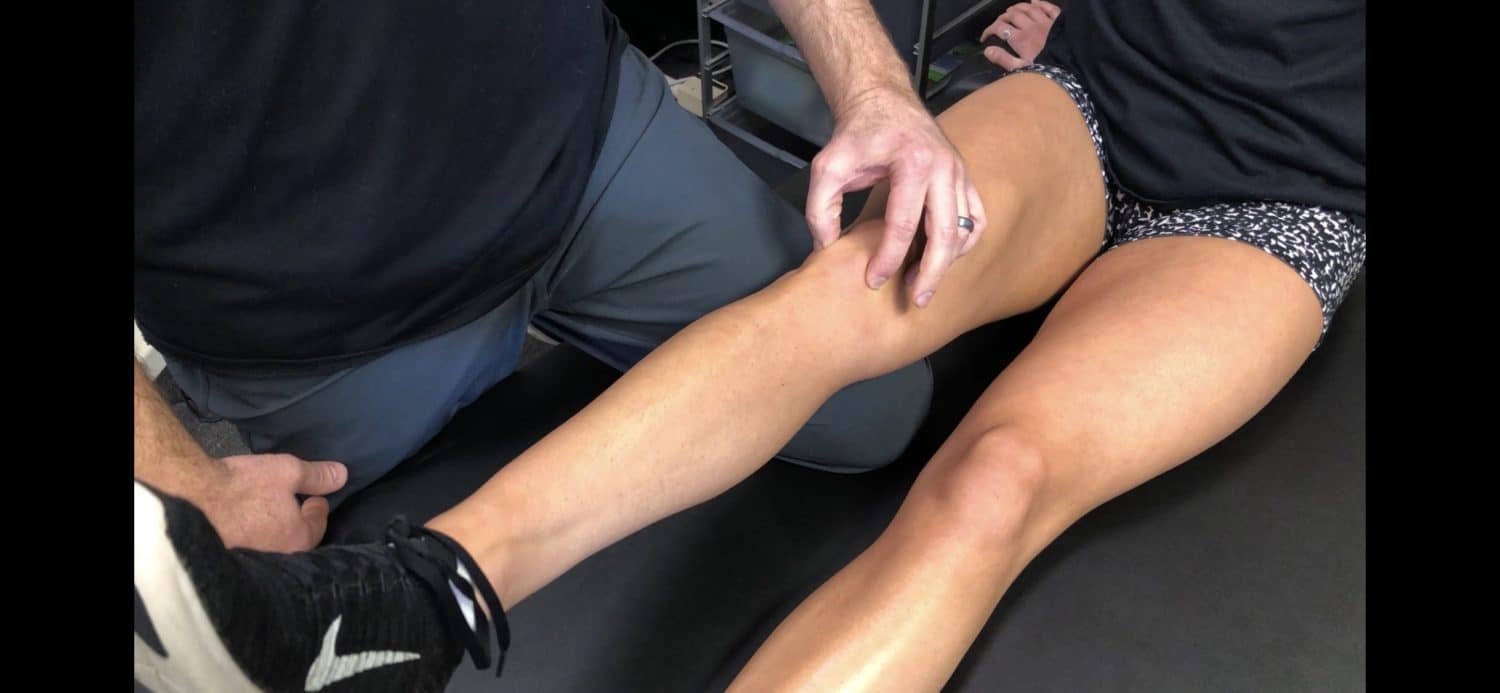
Anterior Knee Pain- A Test for Fat Pad Irritation
We as physical therapists are constantly seeing patients with anterior knee pain with a very vague history. Often times, there’s not a specific onset or mechanism of injury. With that, it seems as if the retro patellar fat pad is a common source of pain in many people and is commonly overlooked. What actually hurts in…
-
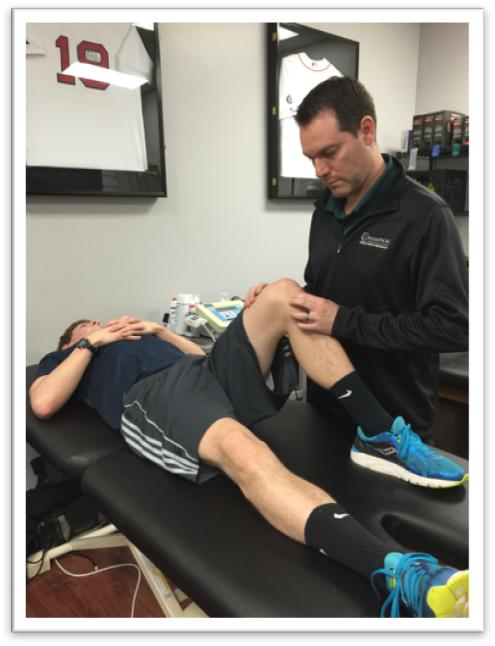
Diagnosing meniscus tears: What’s the literature telling us now?
Meniscal tears are commonly observed in an outpatient physical therapy setting. The ability of a PT to evaluate a patient’s knee and diagnose a meniscus tear can help guide the treatment plan for that patient. Having specific tests that can accurately and quickly pick up a meniscal tear are valuable. Lots of test options but stick…
-
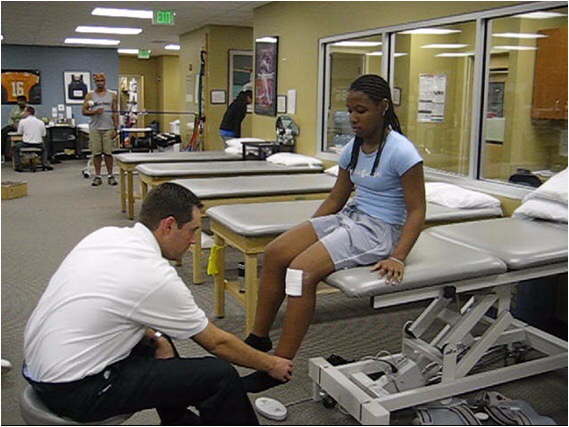
The Challenges of ACL Rehab- It’s Never Easy!
It seems like I always have someone on my schedule that is post-op ACL reconstruction (or anything post-op, for that matter!). Although I thoroughly enjoy progressing ACL rehab because this population is very motivated to get back to their sport or activity. Knowing that it scares the bejeezus out of me at times! There are…
-

Welcome to LennyMacrina.com!
Welcome to my new website, LennyMacrina.com I hope to share some of my insight into the field of physical therapy, rehabilitation, and performance. My goal is very simple: Take a huge step back from the complexities of all of the information on the web and make it more intelligible and applicable to your daily practice.…
-

2 Tips to Improve Your Post-op Rehabilitation Outcomes
I’ve treated hundreds, if not thousands of postoperative patients in my career. I’m always surprised to hear from others how they progress their patients. When I first got into physical therapy, I was all about protocols. I didn’t have much experience. I would literally follow it word for word and do my best to match…