Tag: overuse
-

The Week in Research Review, etc 11-19-18
—
by
Great ‘Week in Research Review, etc 11-19-18’ that I hope you find helpful to your practice. I’ve always touted the importance of the subjective portion of the exam so I wanted to share a slide from a recent talk I gave to a group in Canandaigua, NY. Obviously, the squat is a fundamental movement and…
-

The Week in Research Review, etc 11-12-18
—
by
This week in research review for 11-12-18 we focused a bit more on assessment and also dabbled in some basic treatment strategies for the back and shoulder. Check out the topics below and like them or comment on Instagram to keep the conversation going…thanks all! A quick fix for a sore low back? Knee…
-

The Week in Research Review, etc 10-29-18
—
by
This week we started the week off with a couple shoulder posts, specifically the rotator cuff and SLAP tears. As usual, I can’t resist a good ACL paper so included that NM control program that should be in all knee patients’ programs. We ended the week with a recorded knee scope as the surgeon was…
-
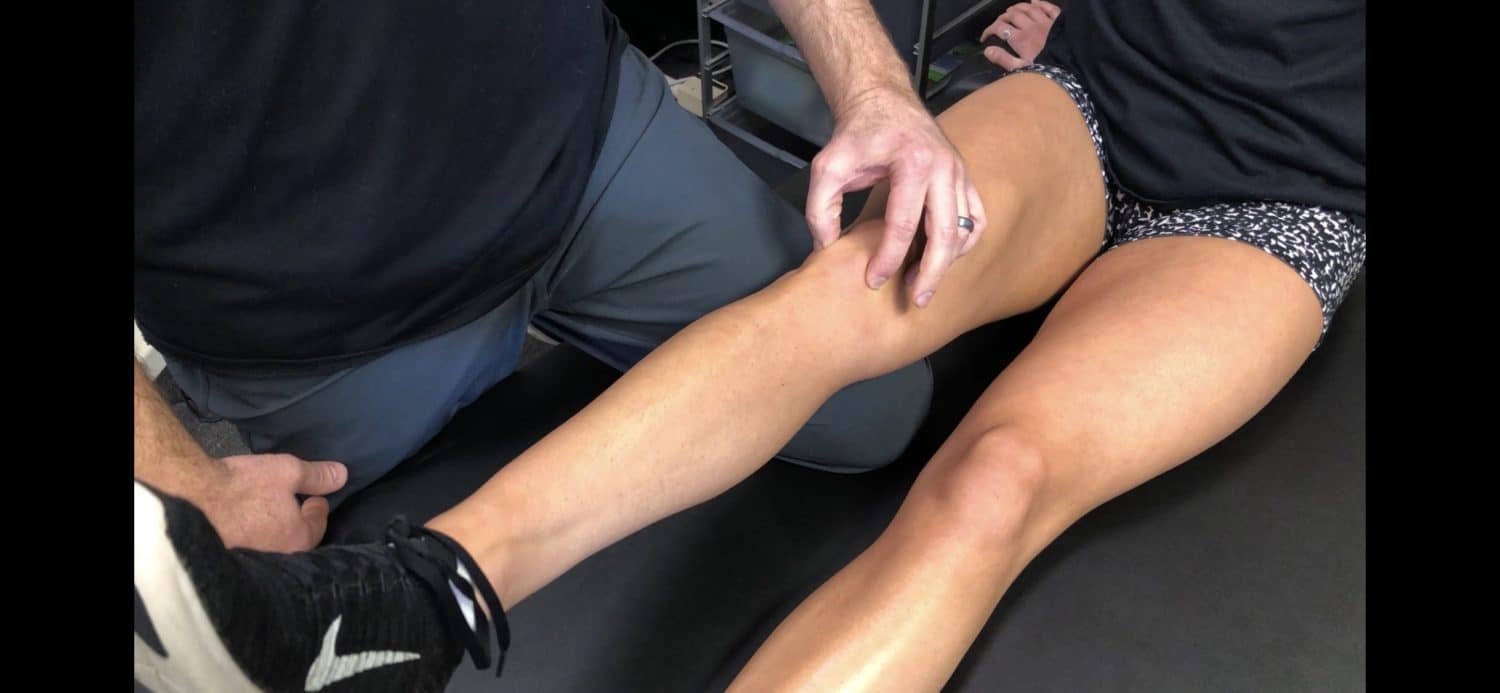
Anterior Knee Pain- A Test for Fat Pad Irritation
We as physical therapists are constantly seeing patients with anterior knee pain with a very vague history. Often times, there’s not a specific onset or mechanism of injury. With that, it seems as if the retro patellar fat pad is a common source of pain in many people and is commonly overlooked. What actually hurts in…
-

Kids and Sports Injuries: What are we doing wrong?
I recently had a conversation with a parent who reached out to me slightly concerned for her 12-year-old child. He’s stressed out, hurt again and she didn’t know if I could help. It made me think about kids and sports injuries… and how we could make a difference. Real Life Story I had seen this…